|
We have all heard about probiotics, and how good they are for us. We have probiotic yoghurts, fermented foods, kefir, and probiotic gum easily available to us. After taking antibiotics, many of us know that it’s a good idea to replenish our good bacteria and load up on probiotics. As a naturopathic doctor, a recommendation for a good quality daily probiotic is very common for most of my patients. However, there is a subpopulation of my patients for which this is NOT a good idea. At least, not initially. These patients actually have an overgrowth of bacteria in the small intestine, and giving them probiotics can actually make them worse if we don’t treat the underlying condition first. Most of these patients have already been diagnosed with Irritable Bowel Syndrome (IBS). However, the diagnosis of IBS doesn’t actually tell them what is causing it, just that their bowel is irritable and that they most likely don’t have a more serious condition. Since I have started testing for it, I have found that many of my IBS patients actually have Small Intestinal Bacterial Overgrowth (SIBO) as the underlying condition. Furthermore, even if you have a diagnosis of Celiac disease, Colitis, or Crohn's, you may still have SIBO: those with these conditions actually have a 3-fold increased risk of developing SIBO, because of all of the gut inflammation, and its effect on the nervous system surrounding the digestive tract. So, what might be some indications that you might have SIBO? 5 Key Clues That May Indicate SIBO 1) Bloated all the time You may start off the day with a relatively flat stomach, but as the day progresses, you go up a few sizes and may look pregnant! This might happen no matter what you eat. Or, you may have identified a few foods that make things worse, but even when you avoid them, you still get some digestive symptoms. 2) You feel worse with high fibre and/or sugary foods A diet high in fibre can lead to increased fermentation of food by bacteria in the small and large intestines, and if you already have an overgrowth of bacteria, you can imagine that this could lead to increased gas. Sugary foods, and/or foods high in certain types of carbohydrates (high FODMAPs foods), also feed the bacterial overgrowth, and can worsen symptoms. And it’s not just bloating that you could experience. Depending on the predominant type of bacteria present, hydrogen-producing of methane producting, you could also experience diarrhea and/or constipation, or even heartburn. 3) You have a history of bacterial gastroenteritis If you’ve had a bad stomach bug, or haven’t been well after “traveller’s diarrhea”, this may have set off the fine balance in your gut and contribute to SIBO. You may have also been put on strong antibiotics, which can kill off some of your good bacteria and allowed less beneficial bacteria to thrive. 4) Your thyroid is sluggish You may have been diagnosed with hypothyroidism, or have sub-laboratory hypothyroidism (your thyroid function may not be slow enough to be prescribed Synthroid for it, but you have symptoms). Either of these can slow down your digestive system and the transit time down the digestive tract, allowing bacteria more time to ferment it. 5) Taking probiotics makes you worse This makes sense, as, if you have an overgrowth of bacteria in the small intestine, populating with more bacteria, even the “beneficial” ones, could make things worse. Not everyone with SIBO gets worse with probiotics, but most SIBO patients don’t feel significantly better on them if we don’t get rid of the overgrowth first and make sure that the sweeping function (migrating motor complex) of the small intestine is working properly beforehand. Does this sound like you? Have you been struggling with ongoing digestive issues but haven’t had a breakthrough yet? Come on in for an assessment, and we’ll see if testing for SIBO would be a good idea for you! References: Image from 123rf.com, Copyright: <a href='https://www.123rf.com/profile_drmicrobe'>drmicrobe / 123RF Stock Photo</a> Khangura, P. (2017). Superseding SIBO. Webinar 2017 May 13.
1 Comment
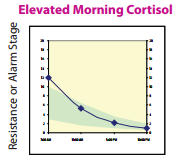
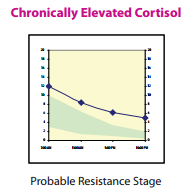
You’re feeling overwhelmed, your body doesn’t listen to you anymore, you’re exhausted but you can’t sleep, you’re gaining weight around the belly, and you have your suspicions that chronic stress is to blame. You may have read my previous blog about adrenal fatigue, and figured that your adrenal glands are likely getting exhausted from working overtime to help you cope in a stressful world. But the symptoms of adrenal fatigue are wide and varied. How can you test and find out how healthy your adrenal glands really are? Furthermore, how do you find out which stage of adrenal fatigue you may be in? Hormonal Questionnaire I use a ranked questionnaire shared by Dr. Tara Scott and Dr. Ken Spiedel at a conference I recently attended, which uses symptom severity and an algorithm to figure out your most predominant hormone imbalances. While this is not a fool-proof test, it allows us to get an idea of what are most likely to be your top 3 hormone imbalances. The results from this simple questionnaire tend to correlate well with the results from hormone testing, helping direct further objective testing. It can help us identify if most of your symptoms are likely from too high cortisol, too low cortisol, both, or something else altogether. In-Office Testing During a physical exam, there are a few specific tests I can do that indicate if you are likely in Stage 3 adrenal fatigue, where your cortisol production goes down. The first test looks at your pupil’s reaction to light. I shine a light in your eye, and see if you can maintain your pupil’s constriction for a short period of time. If you can’t, or your pupil closes and then opens in this time frame, this is one possible indication that your adrenal glands are fatigued, as it correlates with your adrenaline levels (also produced by the adrenal glands). The second test I do in-office is checking your blood pressure lying down, and then standing up (called orthostatic blood pressure). Generally, when you get up, you should be able to bring your blood pressure up by about 10 points within one minute. If it stays the same or goes down, it could be a sign of hypoadrenia. Again, other factors can affect this, including medications that you’re on. This test will likely be positive (blood pressure will stay the same or go down when you get up) if you are in Stage 3 adrenal fatigue. However, if you’re in Stage 1 or Stage 2, or even early Stage 3 adrenal fatigue, this test may still look normal. Salivary Hormone Testing Salivary hormone testing for cortisol and its precursor, DHEA, is the preferred method for testing adrenal function. Cortisol is the main hormone produced by the adrenal glands during chronic stress. There are several advantages of this method over doing a blood test for cortisol: 1) Salivary testing avoids falsely elevating cortisol levels from doing a blood draw. Pricking or lancing has been shown to increase cortisol levels just because of the anxiety the procedure causes for many people, whereas spitting into a tube in the comfort of your own home usually does not. 2) Salivary testing can be done several times throughout the day, allowing us to see the normal (or abnormal) daily variation of cortisol. Blood is not convenient to test more than once during the day. However, cortisol levels usually are highest in the morning, and then decrease during the rest of the day. Seeing where your levels fall at 4 different time points allows us to more accurately assess which stage of adrenal hypo-functioning you may be in.
3) Salivary testing allows us to identify the level of cortisol that is actually getting to your tissues, where it acts (the active cortisol). Blood levels usually use very large “normal” ranges, and include both bound (inactive) and free (active) cortisol. Blood Levels of Cortisol As mentioned above, this is not the preferred method. But, if we want to screen out more serious conditions of the adrenal glands, such as Addison’s Disease (extremely low adrenal function) or Cushing’s Syndrome (abnormally high cortisol), blood tests could be used. Ready To Test? If you suspect your adrenals are near or at burnout, or you are under chronic stress, don’t delay in pursuing treatment with a naturopathic doctor. The health of the adrenal glands is intertwined with that of so many hormones, so make sure you take care of these little soldiers before they’re too exhausted to take care of you! In health, Dr. Tamar References Image from 123rf.com, copyright: <a href='https://www.123rf.com/profile_pixelsaway'>pixelsaway / 123RF Stock Photo</a> Rocky Mountain Analytical (2014). Adrenal Function Panel: Clinical Information for Professionals. January 2014. Scott, TD, Speidel, K. (2017). Essential Elements of Prescription Hormone Compounding. LP3 Network. Conference 2017 Apr 29-30. We all deal with stress. Stressors such as losses, job interviews, presentations, medical diagnoses, lack of sleep, job and home life balance, or challenging relationships can make us feel overwhelmed. Our bodies should be able to deal with these stressors, for a short period of time. And that’s the key: for a short period of time. The problem is, most of us are chronically stressed! How Heavy Is The Burden You Carry? You’ve probably heard of the analogy of holding a glass of water. Hold it for a minute, and it feels light. Hold it for an hour, and your arm will start to ache. Hold it for a day, and your arm will be numb and the glass will feel unbearably heavy. We often don’t remember to put the glass down until it’s too late. Until we have seen the repercussions on our body, mediated primarily by our adrenal glands, these little soldiers that sit on top of our kidneys, trying to fight for us. Fight Or Flight Your adrenal glands perceive any form of stress, whether it is a physical, emotional, environmental, biochemical, or spiritual stress, and respond the same way: by trying to produce either adrenaline (short-term) or cortisol (long-term). They are responsible for our fight or flight response: when our body assesses its environment and deems it unsafe, it prepares us for battle, getting our blood pumping, shifting our resources away from digestion and into our muscles and brain so that we can run from danger or fight it head on. But if this goes on for a long period of time, we will get exhausted, as it’s just not sustainable. How Chronic Stress Affected Me When I graduated from naturopathic medicine, and shortly after writing my licensing exams, my adrenal glands were in rough shape. I had pushed myself through medical school, but once the stressor was over, it was difficult for me to peel myself off the couch or do any exercise at all. I had survived on insufficient sleep, caffeine, deadlines, and willpower, but in the process, my digestion was a mess, and I was constantly battling fatigue throughout the day. Any new stressor made me feel overwhelmed. Luckily, as a new naturopathic doctor, I knew that my adrenal glands were in need of some tender loving care. I was probably near burnout. It took me a good year before I felt a lot better, and a few years more before I felt better than I had years before, during my undergraduate and naturopathic medical school studies. You don’t need to be near breaking point before realizing that your adrenal glands need some help, and that stress is affecting your body in various ways. It’s best to catch it in the early stages, when it’s easier to shift back to balance. Adrenal Fatigue Stages You may have heard of the term “adrenal fatigue” (or adrenal insufficiency, hypoadrenia) from naturopathic doctors and integrative medical doctors. This term really refers to an older concept founded on Dr. Hans Selye’s research (a Canadian endocrinologist), called “General Adaptation Syndrome”. If we are under stress for long enough, we move through the different stages of adaptation to chronic stress, from the alarm stage, to the exhaustion stage. At the end of the exhaustion stage is burnout. You don’t want to get to the exhaustion stage if you can prevent it! Stage 1 – Alarm In this initial alarm stage, the body panics a little and tries to mobilize its resources. You might have a temporary decreased resistance to stress as your body starts to produce more cortisol to deal with the chronic stress, and you mobilize your energy sources from fat and muscle. Some people will lose weight in this stage. Stage 2 – Resistance In this stage, the adrenal glands actually grow in size as they try and keep producing more cortisol. But the high cortisol will wreak havoc on the body. Symptoms of high cortisol include: -feeling tired but wired -anxiety and nervousness; heart palpitations -depressed mood; irritability; mood swings -brain fog, confusion; memory problems; decreased concentration -decreased sex drive -fluid retention -hot flashes; night sweats -hypoglycemia -sleep disturbances -thinning skin -weight gain around the middle -more frequent colds and flus Stage 3 – Exhaustion In this stage, the adrenal glands can’t keep up with the production of cortisol and eventually cortisol production goes down. Any added stressor will be more difficult to deal with, as your resilience goes down. While cortisol levels fluctuate throughout the day, your highest levels of cortisol should be in the morning. Morning cortisol levels are also the last ones to drop in hypo-functioning adrenals. Cortisol helps keep us alert. So if you are having trouble peeling yourself out of bed, and you have late afternoon energy crashes, you may be in this stage. At this stage, you may have symptoms of both low and high cortisol all at once. Symptoms of low cortisol include: -apathy -burned out feeling -anxiety -chemical sensitivities -cold body temperature; cold extremities -cravings for sweets and/or salt -decreased stamina -hypoglycemia -fatigue -joint pains; muscle pains -low blood pressure At the end of naturopathic school, I was definitely into Stage 3. Luckily, there are things we can do to help you deal with the stress and rebuild the health of your adrenal glands. Do you need to put your glass down? Do you think you might suffer from adrenal fatigue? In my next blog, I will discuss testing methods for assessing the health of your adrenal glands, so that you can know which stage you’re in and we can treat more specifically based on your needs. But if you’ve read this and think you’re in the later stages based on your symptoms, don’t wait! Come on in for a visit, and I’d be happy to help you start to feel better. And don’t forget to put your glass down! References Image from 123RF.com, Copyright: https://www.123rf.com/profile_bialasiewicz'>bialasiewicz / 123RF Stock Photo</a> Selye, H. (1998). A Syndrome Produced By Diverse Nocuous Agents. Journal of Neuropsychiatry, Spring 1998; 10(2): 230-231. Scott, TD, Speidel, K. (2017). Essential Elements of Prescription Hormone Compounding. LP3 Network. Conference 2017 Apr 29-30. |
AuthorDr. Tamar Ferreira is a Naturopathic Doctor in Brampton, Ontario. Her areas of focus include digestive health, hormone balance, and skin conditions. Topics
All
Archives
May 2020
|
118 Queen St. W., Suite 205
Brampton, ON
L6X 1A5
905-451-3963




 RSS Feed
RSS Feed