|
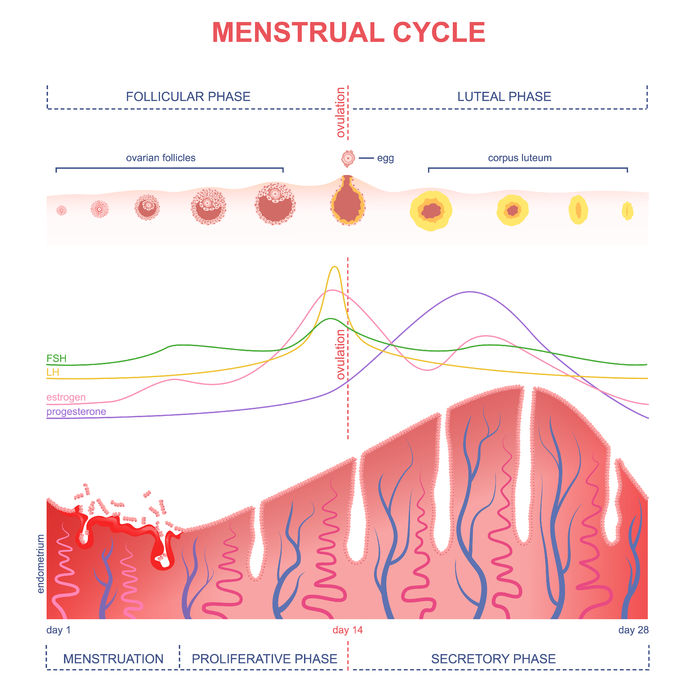
“Doc, I think I have a hormone imbalance.” The majority of the women I see in my practice first come in with some form of hormone-related concern. If they are in their reproductive years, they may suffer from PMS, spotting between periods, painful periods, PCOS, cyclical acne, or irregular periods. In their pre-menopausal years, their period may still come but irregularly, accompanied with hot flashes, insomnia, lowered thyroid function, and other symptoms. Once in menopause, women still experience symptoms related to changes in their hormones. Resolving those imbalances can seem complex and overwhelming at times, but never underestimate the power of what you put at the end of your fork: your food. One of the first dietary tools that I recommend to patients to help balance hormones is called seed cycling. I have seen this alone have a positive impact within 3 months in patients who do just that! Of course, most cases are much more complex and necessitate a multi-pronged approach. But the effectiveness of this simple and low cost therapy as a starting point should not be overlooked. What is Seed Cycling? Seed cycling uses specific estrogen-balancing and progesterone-balancing seeds at different times of your menstrual cycle in order to help shift and improve hormone imbalances. It is as simple as incorporating a total of 2 Tbsp of the specific seed(s) (I usually recommend a raw form) once a day, switching seeds halfway through your cycle, around ovulation. Why do we switch seeds? The beginning of your menstrual cycle is the first day of your period (Day 1). From Day 1 until ovulation (typically around Day 14 IF you have a textbook 28 day cycle), the predominant hormone is estrogen, which helps build up the lining of your uterus (the endometrium) after your period. Flaxseeds and/or pumpkin seeds help to balance estrogen levels and are therefore used in this first half of the cycle. From ovulation until your period starts is the second half of your cycle, in which progesterone is more predominant. This is why we switch to the progesterone-balancing seeds, sesame and/or sunflower seeds. A typical cycle will look like this:
-Day 1-14 (follicular phase): 2 Tbsp (total) of freshly ground flaxseed (or whole pumpkin seeds) – estrogen balancing -Day 15-28 (luteal phase): 2 Tbsp (total) of sesame or sunflower seeds – progesterone balancing You can use a combination of the seeds (1Tbsp of each), or just stick to 2Tbsp of one kind in each category. If your cycle is not 28 days, and/or you have no clue when you ovulate, then you will need to start charting your cycle (using markers such as cervical mucous +/- basal body temperature), in order to find out your particular pattern and whether it falls within the normal range. I like the Kindara App to help with tracking this, but there are many other apps out there, or you can you good old pen and paper charts too! How Does It Work? You might be asking yourself if taking these little seeds daily can really have an impact on your hormones. After all, if you go to your medical doctor to try and “balance hormones”, you will usually be recommended some form of birth control. This actually does not balance your hormones at all, but it suppresses your natural production of hormones in order to try and prevent the process of ovulation, fertilization, and make the uterus lining inhospitable to embryo implantation. Furthermore, the birth control pill sets you up for specific vitamin and nutrient deficiencies, as well as imbalances in your gut flora (the good bugs that help regulate your immune system). Therefore, if your goal is to balance hormones, the birth control pill is not your answer. Although there are no studies of the seed protocol itself, we do know from studies of the individual seeds how they may be gently nudging our hormones in the right direction. -> Flaxseeds Most women tend to have estrogen dominance, too much of the hormone estradiol, which can manifest as fibroids, endometriosis, mood swings, hair loss, breast tenderness during PMS, and even an increased risk of estrogen-positive cancers such as breast and ovarian cancer. Flaxseeds are considered a “phytoestrogen”, but they don’t directly boost all estrogens as the name might lead you to think. They actually decrease the production of the more harmful estrogen form of estradiol, as well as shift the balance of estrogen metabolites (breakdown materials) from the more harmful 16-hydroxy-estrone towards the less harmful 2-hydroxy-estrone. What they are actually “boosting” is the more beneficial estrogen metabolites… Win-win! Ground flaxseeds have been shown to be helpful for premenstrual breast tenderness and to decrease estrogen-dependent cancer risk. -> Pumpkin and Sesame Seeds Similarly to flaxseeds, pumpkin seeds also have phytoestrogens which have shown potential in decreasing estrogen-dependent cancer risk, but they have not been studied as extensively as flaxseeds. Zinc is high in both pumpkin and sesame seeds, and indirectly helps increase your production of progesterone. The corpus luteum (the “shell” that is left over in your ovaries from the egg that is released during ovulation) becomes the main producer of progesterone in the second half of your cycle, but only if you ovulate. Zinc increases progesterone production by stimulating the hormone FSH, which is needed for proper ovulation to occur. -> Sunflower Seeds Sunflower seeds are high in selenium, magnesium, Vitamin B6, Vitamin E, and also contain a decent amount of zinc. These nutrients are needed for proper progesterone production and hormone metabolism. How To Get Started If you are dealing with some female hormone imbalances and would like to get started with this dietary intervention, you can start at any time! Just make sure to find out what phase of your cycle, follicular (1st half) or luteal (2nd half) phase, you are in, and start consuming the seeds for that phase until it’s time to switch. As these seeds are high in fibre, make sure to have them with plenty of water so that you don’t get constipated. As well, some people experience bloating when they start eating these amounts of ground flaxseeds – if this is you, cut back and start small, working your way up, or try pumpkin seeds instead. If your case is more complicated or you have irregular cycles, it might be worth it to get a proper evaluation. You may need an in-depth hormone assessment through bloodwork, salivary hormone testing, or dried urine testing (DUTCH test) to really find out what is going on. Naturopathic doctors have many tools to help you balance your hormones, including dietary and lifestyle changes, botanical medicines, nutritional supplementation, and acupuncture. As always, I would love to help you get to the bottom of your hormone troubles so that you don’t have to fear that time of the month anymore. Make an appointment at my Brampton office to get started. In health, Dr. Tamar References Haggans CJ, Travelli EJ, Thomas W, Martini MC, Slavin JL. The effect of flaxseed and wheat bran consumption on urinary estrogen metabolites in premenopausal women. Cancer Epidemiol Biomarkers Prev. 2000 Jul;9(7):719-25. Images from 123rf.com. Maleki-Saghooni N, Karimi FZ, Behboodi Moghadam Z, Mirzaii Najmabadi K. The effectiveness and safety of Iranian herbal medicines for treatment of premenstrual syndrome: A systematic review. Avicenna J Phytomed. 2018 Mar-Apr;8(2):96-113. Mojgan Mirghafourvand, Sakineh Mohammad-Alizadeh-Charandabi, Parivash Ahmadpour, Yousef Javadzadeh. Effects of Vitex agnus and Flaxseed on cyclic mastalgia: A randomized controlled trial. Complementary Therapies in Medicine; Volume 24, 2016: 90-95. Richter D, Abarzua S, Chrobak M, Vrekoussis T, Weissenbacher T, Kuhn C, Schulze S, Kupka MS, Friese K, Briese V, Piechulla B, Makrigiannakis A, Jeschke U, Dian D. Effects of phytoestrogen extracts isolated from pumpkin seeds on estradiol production and ER/PR expression in breast cancer and trophoblast tumor cells. Nutr Cancer. 2013;65(5):739-45. Sicilia T, Niemeyer HB, Honig DM, Metzler M. Identification and stereochemical characterization of lignans in flaxseed and pumpkin seeds. J Agric Food Chem. 2003 Feb 26;51(5):1181-8. Wzelaki, Magdalena. Seed Cycling to Balance Pre and Post Menopausal Hormones. Dr. Jolene Brighten. 2009-2019. Accessed Jan 22, 2019: https://drbrighten.com/seed-cycling-menopausal-hormones/.
0 Comments
The connection between liver health and the skin is well-known, especially in serious liver diseases. For example, a yellowing of the skin is seen with liver cirrhosis, a condition in which scarring replaces normal functioning liver tissue. Pruritis, or skin itching, can also be associated with liver disease. The reason? The liver is one of the major detoxification organs in the body. It filters the blood and processes, breaks down, and packages major toxins (metabolites, alcohol, caffeine, medications, hormones, environmental pollutants) that your body is exposed to, in order to either make them more usable by the body, or to eliminate them. If this “processing plant” is overburdened and starts to work more sluggishly, the toxins need to go somewhere. Often, in an attempt of the body to get rid of them, many will end up in the skin, a secondary organ of elimination, and also our largest detoxification organ. Even if you don’t have a serious liver disease, your liver enzymes may not be working as optimally as they could, with repercussions showing up elsewhere, such as your skin. Therefore, in order to have healthy-looking skin, you want to make sure that your primary organs of detoxification are working properly. Supporting Your Primary Organs of Detoxification
Our primary organs of detoxification include the liver, the intestines, and the kidneys. 1) Drink Enough Water You can support kidney detoxification by drinking a sufficient amount of water, typically about 2L a day for the average person (preferably mostly away from meals to prevent diluting your digestive enzymes too much). As a rule of thumb, you should be drinking about half your body weight (in lbs) in ounces (i.e. for a 150 pound person, 150/2 = 75 oz, or roughly 9 cups). This helps you eliminate water-soluble toxins from your body, with the added bonus of plumping up your skin and decreasing the visibility of wrinkles. 2) Clean Up Your Diet Reduce foods in your diet that will put more burden on your digestive system and on your liver. This includes processed food and sugar, alcohol, caffeine, and food sensitivities. If you’re not sure about your food sensitivities, book an appointment and I’ll run a simple lab test or help you identify them through an elimination diet. You’ll also want to include foods that help improve liver function, including leafy green vegetables, cruciferous vegetables, berries, turmeric, and sufficient protein. 3) Take Probiotics Probiotics are essential for a healthy gut and immune system. They can be obtained from fermented foods in the diet, but this can be problematic since many people with skin conditions cannot tolerate cow’s dairy, including regular yoghurt. An alternative yoghurt, such as sheep or goat yoghurt, could be an option if they are better tolerated. However, probiotic supplements may be your best option. With supplements, we can be specific about which strains of probiotics we are using, as each strain has a slightly different effect on the immune system. For example, I use a different blend with a patient with acne versus someone suffering from an autoimmune condition such as psoriasis. 4) Drink Lemon Water One simple addition you can try at home that gently supports liver function is starting the day with a large glass of lemon water (about 500mL of water with the juice of about ¼ of a lemon). You’ll want to wait about half an hour before having your breakfast afterwards. Again, you don’t want to dilute your digestive enzymes! 5) Use Nutraceuticals To Support Liver Detoxification With many skin conditions, including acne and eczema, I see the fastest improvement when we include some liver supporting herbs and nutrients into the treatment plan. These can include high quality, concentrated extracts of milk thistle, dandelion, turmeric, B vitamins, and other nutraceuticals. Because these supplements can interfere with medications you are taking, or could have side-effects, work with a naturopathic doctor who can recommend the best avenue for you, monitor your progress, and modify your treatment plan if necessary. A word of caution: liver supporting herbs can initially worsen a skin condition, especially if the intestines are not working well, or if you start too much, too quickly. Do you want healthy, glowing skin from the inside out? Then making sure that your body’s primary organs of detoxification are working to your full advantage is extremely important. I can help you identify your food sensitivities, heal your digestive system, and support proper liver detoxification through an individualized program tailored to your specific needs. If you’ve dealt with a skin condition, such as acne or eczema, you’ve probably tried a series of different skin regimens to help improve your skin. I know what it’s like. I’ve been there, struggling with eczema, which ultimately led me to a career change from biochemical research to naturopathic medicine. You see, no matter how much I diligently used my cortisone creams and moisturizers, it kept coming back, and I knew I needed to look deeper for the answers. I found the answers were not merely skin deep. The answers were in my gut!
Naturopathic medicine has long taught that skin conditions need to be addressed through the health of the gut, and that the gut and the skin are intimately connected. When you think about it, the inside of your digestive system is like an internal continuation of your external skin. We now know that a huge part, about 80%, of your immune system lies in your gut, and that many skin conditions are associated with a dysregulation of the immune system. Your gut is your first line of defense against pathogens, and regulates your immune system’s response to different foods, toxins, and micro-organisms. To have healthy skin from the inside out, you must first address the health of your gut! This is primarily how I address skin conditions in my practice, from the inside out, and I have seen great improvements in my patients’ skin conditions using this approach. Skin Conditions Associated With Digestive Issues If the link between digestive issues and skin conditions is real, we would expect to see a strong correlation between digestive diseases and skin conditions. And we do see this. For example: -Acne rosacea, an inflammatory condition of the skin on the face, is associated with a higher prevalence of gastrointestinal complaints (including Celiac disease, Crohn’s Disease, Ulcerative Colitis, H. pylori infection, Small Intestinal Bacterial Overgrowth (SIBO), and Irritable Bowel Syndrome (IBS)) than in the general population (Egeberg et al., 2017). -Eczema and other rashes have been associated with reactions to certain foods, including in a condition called Non-Celiac Gluten Sensitivity (Elli et al., 2015). -Dermatitis herpetiformis is a skin condition found in ¼ of patients with Celiac disease (Kresser, 2012) The Leaky Gut, Leaky Skin Connection We now know that chronic inflammation and damage to the gut lining can lead to a state of intestinal hyperpermeability, where food particles and microbial toxins that shouldn’t get through do get through, leading to what we call a “leaky gut”. This damage could happen as a result of many things, including food sensitivities, genetically modified foods, an imbalance in gut flora (the microbes in the gut), infections, and chronic stress. Many of these things worsen skin conditions as well. Stress not only impacts the gut barrier, it also makes the skin barrier more permeable, which is why you may experience a worsening of your skin condition when you are particularly stressed (Slominski, 2007). If the gut is leaky, this also influences the immunity of the skin, making it produce less protective anti-microbial peptides. Another aspect of the gut-skin connection, which I will address in a later blog, has to do with detoxification. If the gut, a primary organ of detoxification, is compromised, then the body will try and detoxify through other means, including the secondary detoxification systems, which includes the skin. Treating The Gut Improves The Skin Treating skin conditions definitely requires a multi-faceted approach. However, in my practice and in my own personal experience with eczema, I have seen a tremendous improvement in skin conditions by addressing the health of the gut first and foremost. For example, including probiotics in the diet, either through fermented dairy or through probiotics, can significantly improve the severity of acne vulgaris. Treating SIBO in a patient with acne rosacea is likely to improve their rosacea symptoms. Removing gluten in the diet usually resolves dermatitis herpetiformis. So why just stick to skin deep treatments when you can address the root cause(s) of your skin condition? Changing my diet and healing my leaky gut has been extremely important in helping me minimize my eczema. A similar approach has helped countless of my patients, and I’d love to help you too! References Egeberg A., Weinstock L.B., Thyssen E.P., Gislason G.H., Thyssen J.P. (2017). Rosacea and gastrointestinal disorders: a population-based cohort study. Br J Dermatol., 2017 Jan;176(1):100-106. doi: 10.1111/bjd.14930. Elli L., Branchi F., Tomba C., Villalta D., Norsa L., Ferreti F., Roncoroni L., Bardella M.T. (2015). Diagnosis of gluten related disorders: Celiac disease, wheat allergy and non-celiac gluten sensitivity. World J Gastroenterol., 2015 Jun 21;21(23):7110-7119.doi: 10.3748/wjg.v21.i23.7110 Kresser C. (2012). The gut-skin connection: how altered gut function affects the skin. Chris Kresser. Retrieved from: https://chriskresser.com/the-gut-skin-connection-how-altered-gut-function-affects-the-skin/ Slominski A. (2007). A nervous breakdown in the skin: stress and the epidermal barrier. J Clin Invest. 2007 Nov 1; 117(11): 3166–3169. doi: 10.1172/JCI33508 Most women that I see in my practice who are in their reproductive years suffer from premenstrual syndrome (PMS) to some extent. Actually, about 75% of women in this demographic experience PMS (Medline Plus, 2016). Does that make it normal? While a low level of discomfort can be expected (after all, there are huge hormonal changes occurring all at once within the week before your period), in many cases, more severe symptoms are pointing to underlying hormone imbalances or deficiencies that should be addressed. What Is PMS? PMS is generally defined as a group of symptoms that comes and goes cyclically based on where a woman is in her menstrual cycle. They usually will start in the second half of the cycle (at least 14 days after the start of a period in a woman with a textbook 28 day cycle), and will go away 1-2 days after menstruation starts (Medline Plus, 2016). Typical PMS symptoms can include one or more of the following:
-Bloating and/or increased gas -Breast tenderness -Changes in bowel movements, such as constipation or diarrhea -Headaches -Food cravings -Mood changes, such as heightened emotions, irritability, anxiety, or depression -Fatigue -Skin changes, such as cyclical acne Paying attention to these sometimes subtle changes can give you a clue about what imbalances you may have. The 4 Main Types Of PMS PMS is classified into 4 main types. If you fit primarily into one of these 4 main types, your naturopathic doctor will be able to gain valuable insight just from your symptoms! 1) PMS-A (Anxiety): This type of PMS is characterized by symptoms of increased anxiety, irritability, and emotional lability. What it means: PMS-A is usually associated with a high estrogen to progesterone ratio. Think of progesterone as the calming hormone between the two. If you don’t have enough of the calming hormone, estrogen will trigger the release of the more stimulating hormones, cortisol and adrenaline, which will make you feel more on edge. As well, if you’re on or have taken birth control pills in the past, you may have excess estrogen in your system, which can worsen these symptoms. Treatment options: Using natural strategies to increase progesterone (such as the herb Chaste Tree), get rid of excess estrogen, and decrease stress is very helpful for PMS-A sufferers. Increasing magnesium intake can also be helpful. If you have severe PMS-A symptoms, and especially if you are peri-menopausal, you may benefit from cyclical use (post ovulation) of bio-identical progesterone cream (which I can prescribe). 2) PMS-C (Cravings): If you experience strong cravings the week before your period, especially carbohydrate cravings, then you are probably suffering from PMS-C. You may also crave stimulants and chocolate, get heart palpitations, and you may get headaches and energy highs and lows from fluctuating blood sugar levels. What it means: These symptoms are thought to be due to changes in the way insulin binds. As a response to blood sugar in your bloodstream, your body produces insulin as a signal to bring the sugar into the cells. However, in the days leading up to a period, a woman’s cells become less sensitive to this insulin signal, leading to imbalances in blood sugar regulation. Giving in to sugar cravings can actually make PMS-C symptoms worse, since the body can’t deal with this influx of sugar properly. Treatment options: Stabilizing blood sugar with a high protein diet low in refined carbohydrates is really important if you suffer from PMS-C. These blood sugar imbalances can also show up as acne in the skin, since high sugar in the blood can lead to more breakouts. Eat small and frequent meals, and avoid alcohol. 3) PMS-D (Depression): If you feel really down before your period, you don’t feel like participating in your regular social activities, you feel grumpy, angry, or have crying spells before your period, you may suffer from PMS-D. If you have pre-existing depression, you might feel like your symptoms are worse leading up to your period. Another feature of this type of PMS is that it may be associated with premenstrual acne. What it means: The etiology of this type of PMS is like the reverse of PMS-A, with elevated progesterone levels, and low estrogen levels. While progesterone decreases anxiety, too much progesterone relative to estrogen can depress the nervous system, leading to symptoms of depression. As well, the happy neurotransmitter serotonin is decreased when estrogen levels are low, worsening feelings of depression. There also may be elevated testosterone levels, which can lead to increased acne. Treatment options: Some foods and herbs with phytoestrogenic activity can be used to balance estrogen levels. As well, if you have elevated androgens (hormones such as testosterone and DHT), these can be balanced using natural therapies. Including foods high in tryptophan (the precursor to the feel good hormone, serotonin) can help with mood: sour cherries, turkey, cottage cheese, and oats are all high in tryptophan (Pope, 2016). 4) PMS-H (Hyperhydration): If you routinely gain a few pounds before your period, your abdomen feels swollen, or your breasts get more swollen and tender, you are likely suffering from PMS-H. Rings on your hands may feel tighter if it also affects your extremities. What it means: The increased extracellular fluid which leads to symptoms of fluid retention is due to higher aldosterone levels. Aldosterone is a hormone produced by the adrenal glands that helps the body retain fluid. This can be compounded with lower dopamine levels typical in the days leading up to the period. Treatment options: Eating foods high in salt makes the body retain more water, so decreasing your salt intake and processed foods can help decrease the fluid retention. Increasing magnesium intake can also help reduce aldosterone levels and improve symptoms. What’s A Girl To Do? If you are tired of dealing monthly with your PMS symptoms, there is a better way than just pushing through it. Prominent PMS symptoms are signs for you to pay attention to the subtle imbalances in your body. The above treatment options will work for some but must be adapted to your particular case. Naturopathic doctors can help you balance your hormones with tools such as liver supporting and hormone balancing herbs, nutritional supplements, dietary changes, and acupuncture. In more complicated cases, we may need to run hormonal testing (blood or salivary) to find out exactly what we’re dealing with. If you want to get to the bottom of your PMS, I’d love to help. You can get in touch here. References: Image from: http://www.123rf.com/profile_rodimovpavel'>rodimovpavel / 123RF Stock Photo Kaslow JE (2016). Premenstrual Syndromes. Jeremy E. Kaslow, MD. Retrieved from http://www.drkaslow.com/html/premenstrual_syndromes.html. Pope N (2016). Naturopathic Infertility Treatments Timed With Cycle Charting. Webinar May 15, 2016. White CD (2016). Premenstrual Syndrome. Medline Plus. Retrieved from https://medlineplus.gov/ency/article/001505.htm.  If you’re wandering down any typical grocery store, you will usually come across one isle or two promising “freedom” from some of the typical things most people eat: gluten-free, dairy-free, egg-free, soy-free, and the list goes on. You may have wondered if those foods are healthier, and if you should also be filling your grocery cart in that isle. Food sensitivities and allergies are on the rise in North America. It’s hard to plan a kids’ party without someone having some dietary restrictions. So, what’s the difference between food sensitivities, intolerances, and allergies? Food Allergies Most people with food allergies found out the hard way. They ate some peanuts and had difficulty breathing, or ate some strawberries and broke out in hives. These reactions are usually severe, and are mediated by a type of antibody called IgE (antibodies are produced in the body and attach to specific protein sequences that they recognize). If you went to an allergist and got pricks in your forearms, you were most likely tested for IgE reactions. Symptoms of food allergies usually show up fast, usually starting within 15min of consuming the food, and can be quite severe. They are the type of food reaction that is usually immediate, and are associated with anaphylaxis. If you have a food allergy, you have to be very careful about avoiding even trace amounts of the food in question. Food Sensitivities Food sensitivities are typically harder to pinpoint than food allergies, so many people go undiagnosed for years. They are delayed reactions to food mediated by a different type of antibody, IgG. Symptoms occur most commonly within the first day of eating a food, but can occur up to 3 days after. The symptoms of a food sensitivity tend to be more subtle than a food allergy. They can include: -digestive issues (bloating, gas, diarrhea, constipation, etc.) -foggy thinking -feeling like food “just sits there” and doesn’t digest well -migraine headaches -fatigue -difficulty losing weight -skin issues (acne, eczema, psoriasis) -behavioural issues in children Food sensitivities can be identified either through an elimination diet, or through IgG food sensitivity testing. Many patients opt for IgG food sensitivity testing to get a more objective starting point of which foods to start eliminating. This involves a simple blood test that will look at the level of IgG produced with respect to 120-200 foods. However, food sensitivity testing is still controversial. It is not 100% accurate, must be interpreted in the light of what is going on with the patient, and possible cross-reactions (i.e. shellfish IgG can show up high in someone with a dust allergy because the body recognizes a similarity between them). False positives can occur if the patient has a condition referred to as leaky gut syndrome (where the bowels are hyper-permeable and allow too many undigested foods through). False negatives can occur if you have not been eating a certain food, so it is better to do the testing before you start eliminating foods from your diet. In research studies, IgG-based elimination diets have been found to help with: -both migraines and irritable bowel (Aydinlar et al., 2013) -IBS (Drisko et al., 2006; Atkinson et al., 2004) -Crohn’s disease (Bentz et al., 2010) Despite the lack of conclusive research, I have found the test to be very clinically relevant in practice: most of my patients with the relevant symptoms improve quite dramatically when we remove their food sensitivities from their diet. Food Intolerances Reading through articles can be confusing, since the term “food sensitivities” and “food intolerances” is often used interchangeably. However, food intolerances are non immune-mediated reactions to food (no antibodies are involved). Typically, the body will lack something which will make it intolerant to a food. A common food intolerance is lactose intolerance, where one cannot tolerate lactose-containing dairy products because he/she lacks the lactase enzyme in the digestive tract necessary to break down lactose. With lactose intolerance, symptoms usually occur within 30min of consuming lactose, leading to stomach cramps, abdominal pain, and diarrhea. An elimination diet can help identify both food sensitivities and food intolerances. It may take some further testing after that to identify if, for example, your reaction to dairy is due to a sensitivity or an intolerance. What To Do About Them Once you identify which foods are a problem for you, there are healthy and not-so-healthy ways to eliminate them from your diet. Many of the specialty foods free of common allergens/sensitivities are highly processed, and contain fillers, emulsifiers, and sugars to make the texture or flavour more similar to their regular counterparts. Your best bet is to stick with whole foods that are minimally processed most of the time, and only have the processed ones as an exceptional treat. You may also need additional supplements to help heal your gut barrier so that you can potentially tolerate your sensitivities more in the future. Do you think you may have a reaction to a food you are consuming? If you have any questions or would like to get started on an elimination diet or IgG food sensitivity testing, please contact us and we'll help you out! References
Atkinson W1, Sheldon TA, Shaath N, Whorwell PJ.Gut. Food elimination based on IgG antibodies in irritable bowel syndrome: a randomised controlled trial. Gut. 2004 Oct;53(10):1459-64. Aydinlar EI1, Dikmen PY, Tiftikci A, Saruc M, Aksu M, Gunsoy HG, Tozun N. IgG-based elimination diet in migraine plus irritable bowel syndrome. Headache. 2013 Mar;53(3):514-25. Bentz S1, Hausmann M, Piberger H, Kellermeier S, Paul S, Held L, Falk W, Obermeier F, Fried M, Schölmerich J, Rogler G Clinical relevance of IgG antibodies against food antigens in Crohn's disease: a double-blind cross-over diet intervention study. Digestion. 2010;81(4):252-64. Drisko J1, Bischoff B, Hall M, McCallum R. Treating irritable bowel syndrome with a food elimination diet followed by food challenge and probiotics. J Am Coll Nutr. 2006 Dec;25(6):514-22. Images from 123RF.com Go to most dermatologists for acne problems, and most of the time, your diet will not even be addressed. However, the evidence is growing to suggest that what you ingest does indeed affect acne severity. In clinical practice, I have seen dramatic changes in patients’ skin by eliminating certain foods, improving diet, and correcting nutritional deficiencies.
Particular culprits, other than processed foods, appear to be milk and sugar. Since cow’s milk is designed to stimulate growth in newborn cows, it is high in anabolic steroids and growth factors which increase the production of androgens (like testosterone), which in turn stimulate acne growth. Sugar also has an effect on androgen production, although indirectly. It stimulates the production of insulin and insulin-like growth factor, which in turn also promote the production of acne-stimulating androgens. This applies not only to plain sugar, but to foods that convert easily to sugar when eaten (high glycemic index), such as white breads and rice, as well as sugary fruits such as bananas. If you find yourself struggling with acne-prone skin, consider having a closer look at your diet to see if the common culprits, milk and sugar, abound. |
AuthorDr. Tamar Ferreira is a Naturopathic Doctor in Brampton, Ontario. Her areas of focus include digestive health, hormone balance, and skin conditions. Topics
All
Archives
May 2020
|
118 Queen St. W., Suite 205
Brampton, ON
L6X 1A5
905-451-3963







 RSS Feed
RSS Feed